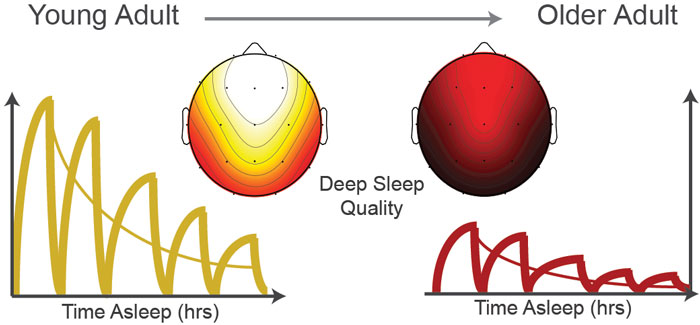
New research shows deeper sleep is crucial for older people Credit: University of California Berkeley
The older you get the deeper sleep you may need, according to new research.
University of California Berkeley researchers believe that the unmet sleep needs of the elderly elevate their risk of memory loss and a wide range of mental and physical disorders.
“Nearly every disease killing us in later life has a causal link to lack of sleep,” Matthew Walker, a UC Berkeley professor of psychology and neuroscience and the paper’s senior author, said in a statement. “We’ve done a good job of extending life span, but a poor job of extending our health span.
“We now see sleep, and improving sleep, as a new pathway for helping remedy that.”
Unlike cosmetic markers of aging, including wrinkles and gray hair, sleep deterioration has been linked to conditions like Alzheimer’s disease, heart disease, obesity, diabetes and stroke.
However, older people are less likely than younger cohorts to notice and report mental fogginess and other symptoms of sleep deprivation, numerous brain studies reveal how poor sleep leaves them cognitively worse off.
Also, the shift from deep, consolidated sleep in youth to fitful, dissatisfying sleep can start as early as a person’s 30’s, leading to sleep-related cognitive and physical ailments in middle age.
In the review of sleep research Walker and fellow researchers Bryce Mander and Joseph Winer cite studies that show that aging brain has trouble generating the kind of slow brain waves that promote deep curative sleep, as well as the neurochemicals that help us switch stably from sleep to wakefulness.
“The parts of the brain deteriorating earliest are the same regions that give us deep sleep,” Mander, a postdoctoral researcher in Walker’s Sleep and Neuroimaging Laboratory at UC Berkeley, said in a statement.
Aging typically brings on a decline in deep non-rapid eye movement or slow wave sleep and the characteristic brain waves associated with it, including both slow waves and faster bursts of brain waves known as sleep spindles.
Youthful, healthy slow waves and spindles help transfer memories and information from the hippocampus, which provides the brain’s short-term storage to the prefrontal cortex, which consolidates the information, acting as the brain’s long-term storage.
“Sadly, both these types of sleep brain waves diminish markedly as we grow old, and we are now discovering that this sleep decline is related to memory decline in later life,” Winer, a doctoral student in Walker’s lab said in a statement.
Elderly people also suffer from the inability to regulate neurochemicals that stabilize sleep and help transition from sleep to waking states. These neurochemicals include galanin, which promotes sleep and orexin, which promotes wakefulness. A disruption to the sleep-wake rhythm commonly leaves older adults fatigued during the day but frustratingly restless at night, according to Mander.
The researchers are examining non-pharmaceutical interventions to boost the quality of sleep, including electrical stimulation to amplify brain waves during sleep and acoustic tones that act like a metronome to slow brain rhythms.
“The American College of Physicians has acknowledged that sleeping pills should not be the first-line kneejerk response to sleep problems,” Walker said. “Sleeping pills sedate the brain, rather than help it sleep naturally.
“We must find better treatments for restoring healthy sleep in older adults, and that is now one of our dedicated research missions.”




