By Mary Beth Gallagher | Department of Mechanical Engineering
The shortage of personal protective equipment (PPE) available to health care professionals has become increasingly problematic as COVID-19 cases continue to surge. The sheer volume of PPE needed to keep doctors, nurses, and their patients safe in this crisis is daunting — for example, tens of millions of disposable face shields will be needed nationwide each month. This week, a team from MIT launched mass manufacturing of a new technique to meet the high demand for disposable face shields.
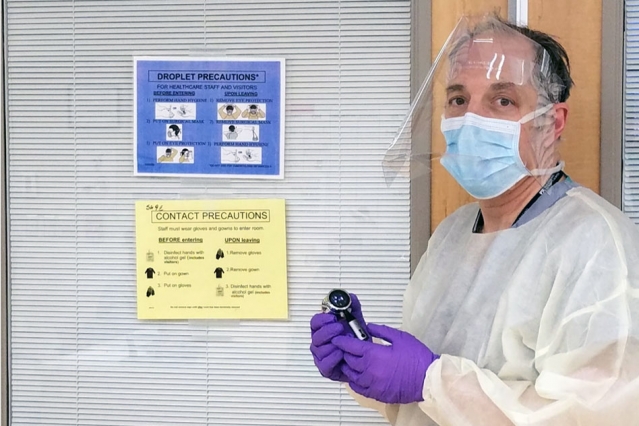
Elazer Edelman, the Edward J. Poitras Professor in Medical Engineering and Science at MIT, wears a face shield developed through a collaborative effort involving groups across MIT, while holding an electronic, Bluetooth-enabled stethoscope. In this photo, Edelman is wearing the shield in the snapped up position health care workers also have the option to use. Image: Elazer Edelman
The single piece face shield design will be made using a process known as die cutting. Machines will cut the design from thousands of flat sheets per hour. Once boxes of these flat sheets arrive at hospitals, health care professionals can quickly fold them into three-dimensional face shields before adjusting for their faces.
“These face shields have to be made rapidly and at low cost because they need to be disposable,” explains Martin Culpepper, professor of mechanical engineering, director of Project Manus, and a member of MIT’s governance team on manufacturing opportunities for COVID-19. “Our technique combines low-cost materials with a high-rate manufacturing that has the potential of meeting the need for face shields nationwide.”
Culpepper and his team at Project Manus spearheaded the development of the technique in collaboration with a number of partners from MIT, local-area hospitals, and industry. The team has been working closely with the MIT Medical Outreach team and the Crisis Management Unit established by Vice President for Research Maria Zuber and directed by Elazer R. Edelman, the Edward J. Poitras Professor in Medical Engineering and Science at MIT.
Extending the life of face masks
When used correctly, face masks should be changed every time a doctor or nurse treats a new patient. However, over the past month, many health care professionals have been asked to wear one face mask per day. That one mask could carry virus particles — potentially contributing to the spread of Covid-19 within hospitals and endangering health care professionals.
“The lack of adequate protective equipment or the idea of reusing potentially contaminated equipment is especially frightening to health care workers who are putting their lives, and by extension the lives and well-being of their families, on the line every day,” explains Edelman, who is also the director of MIT’s Institute for Medical Engineering and Science (IMES) and leader of MIT’s PPE task force.
Face shields can address this problem by providing another layer of protection that covers masks and entire faces while extending the life of PPE. The shields are made of clear materials and have a shape similar to a welder’s mask. They protect the health care professional and their face mask from coming in direct contact with virus particles spread through coughing or sneezing.
“If we can slow down the rate at which health care professionals use face masks with a disposable face shield, we can make a real difference in protecting their health and safety,” explains Culpepper.
Culpepper and his team at Project Manus set out to design a face shield that could be rapidly produced at a scale large enough to meet the growing demand. They landed on a flat design that people could quickly fold into a three dimensional structure when the shield was ready for use. Their design also includes extra protection with flaps that fold under the neck and over the forehead.
As much of MIT’s campus came to a halt in light of social distancing measures being put in place, Culpepper started prototyping using a laser cutter he had in his house. Along with some design input from his children, he tested different materials and made the first 10 prototypes at home.
“When you’re thinking of materials, you have to keep supply chains in mind. You can’t choose a material that could evaporate from the supply chain. That is a challenging problem in this crisis,” explains Culpepper. After testing a few materials that cracked and broke when bent, the team chose polycarbonate and polyethylene terephthalate glycol – known more commonly as PETG – as the shield’s material.
In addition to making more prototypes at the Project Manus Metropolis Makerspace using a laser cutter, Culpepper worked with Professor Neil Gershenfeld and his team at MIT’s Center for Bits and Atoms (CBA) on rapid-prototyping designs for testing using a Zund large-format cutter.
Gershenfeld’s team at CBA is working on a number of projects for coronavirus response using its digital fabrication facility at MIT as well as the global Fab Lab network it launched. “The coronavirus response site is a great resource for those that are interested in working on solutions for PPE and devices for the COVID-19 pandemic,” Culpepper adds.
“It’s been a pleasure in this difficult time collaborating with such an impressive group, drawing on all of the Institute’s strengths to quickly define and refine a solution to an urgent need,” says Gershenfeld. “The work at MIT will be valuable beyond its immediate local impact, as a best-practices reference for the many other face shield projects emerging around the world.”
Testing the shield at local hospitals
With a number of working prototypes built, Culpepper and his team moved to the testing phase after consultation with, and practical feedback from, Edelman, who is also a physician.
“The single greatest insecurity of a health care provider is the thought that we will become infected and in doing so be unable to perform our duties or infect others,” adds Edelman.
Edelman demonstrated how to store, assemble, and use the face shields for nurses and physicians at a number of area hospitals. Participants were then asked to use them in real-life situations and provide feedback using a one-page survey.
The feedback was overwhelmingly positive — participants found that in addition to being easy to assemble and use, the MIT-designed shields provided good protection against coming in contact with virus particles through splashes or aerosolized particles.
Armed with this feedback, Culpepper’s team made a few minor adjustments to the design to maximize coverage around the sides and neck of users. With the design finalized, the project has this week shifted to high-rate mass manufacturing.
High-rate mass manufacturing
The die cutter machines used in mass manufacturing will produce the flat face shields at a rate of 50,000 shields per day in a few weeks. The manufacturer will continue to ramp up and increase the rate of manufacturing further with the ability to fabricate in more than 80 facilities nationwide.
“This process has been designed in such a way that there is the potential to ramp up to millions of face shields produced per day,” explains Culpepper. “This could very quickly become a nationwide solution for face shield shortages.”
MIT plans on purchasing the first 40,000 face shields to donate to local Boston-area hospitals this week and the fabrication facilities will donate 60,000.
“Having an adequate and perhaps even endless supply of PPE is absolutely critical to ensuring the safety of the entire population, especially those who care for Covid-19 patients,” adds Edelman.
Throughout the process, Culpepper’s team received help from a number of colleagues and departments across MIT. This includes MIT’s Office of the Vice President for Research, Professor Elazer Edelman, Tolga Durak, managing director of the MIT Environment, Health and Safety Office, the Center for Bits and Atoms, MIT Procurement Operations, MIT’s Office of the General Counsel, MIT’s Department of Mechanical Engineering, and colleagues from MIT Lincoln Laboratory, who helped source material to build the face shields and supported design iterations. They also received advice from MIT colleagues working with the Massachusetts Technology Collaborative, which is helping organize manufacturers for COVID-19 response.
“This project was a great example of collaboration across MIT and the employment of mind-heart-hand. When we reached out to others, they dropped everything to put their minds and hands to work helping us make this happen quickly,” says Culpepper. “It is also a great example for others to look to safely and rapidly innovate PPE for COVID-19.”





Tell Us What You Think!