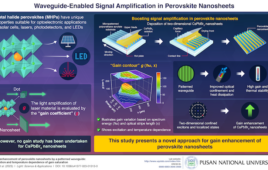
Schematic shows how fluids containing ovarian cancer cells could be removed from the body, treated with magnetic nanoparticles to remove the cells, then returned to the body. Credit: Ken Scarberry |
A paper published in the January issue of the journal Nanomedicine
could provide the foundation for a new ovarian cancer treatment option—one that
would use an outside-the-body filtration device to remove a large portion of
the free-floating cancer cells that often create secondary tumors.
Researchers at the Georgia Institute of Technology have formed a startup
company and are working with a medical device firm to design a prototype
treatment system that would use magnetic nanoparticles engineered to capture
cancer cells. Added to fluids removed from a patient’s abdomen, the magnetic
nanoparticles would latch onto the free-floating cancer cells, allowing both
the nanoparticles and cancer cells to be removed by magnetic filters before the
fluids are returned to the patient’s body.
In mice with free-floating ovarian cancer cells, a single treatment with an
early prototype of the nanoparticle-magnetic filtration system captured enough
of the cancer cells that the treated mice lived nearly a third longer than
untreated ones. The researchers expect multiple treatments to extend the
longevity benefit, though additional research will be needed to document that—and
determine the best treatment options.
“Almost no one dies from primary ovarian cancer,” said John
McDonald, a professor in Georgia Tech’s School
of Biology and chief research
scientist of Atlanta’s
Ovarian Cancer Institute. “You can remove the primary cancer, but the
problem is metastasis. A good deal of the metastasis in ovarian cancer comes
from cancer cells sloughing off into the abdominal cavity and spreading the
disease that way.”
The removal system being developed by McDonald and postdoctoral fellow Ken
Scarberry—who is also CEO of startup company Sub-Micro—should slow tumor
progression in humans. It may reduce the number of free-floating cancer cells
enough that other treatments, and the body’s own immune system, could keep the
disease under control.
Prof. John McDonald (standing) and postdoctoral fellow Ken Scarberry examine statistical data from their study of a potential new treatment option for ovarian cancer. Credit: Gary Meek |
“If you can reduce metastasis, you can improve the lifespan of the
person with the disease and get a better chance of treating it
effectively,” said McDonald. “One goal is to make cancer a chronic
disease that can be effectively treated over an extended period of time. If we
can’t cure it, perhaps we can help people to live with it.”
Earlier in vitro studies published by the authors of the Nanomedicine
paper showed that the magnetic nanoparticles could selectively remove human
ovarian cancer cells from ascites fluid, which builds up in the peritoneal
cavities of ovarian cancer patients. The nanoparticles are engineered with
ligands that allow them to selectively attach to cancer cells.
The researchers believe that treating fluid removed from the body avoids
potential toxicity problems that could result from introducing the nanoparticles
into the body, though further studies are needed to confirm that the treatment
would have no adverse effects.
The recently reported study in Nanomedicine used three sets of
female mice to study the benefit of the nanoparticle-magnetic filtration system.
Each mouse was injected with approximately 500,000 murine ovarian cancer cells,
which multiply rapidly—each cell doubling within approximately 15 hours.
In the experimental group, the researchers—who included research scientist
Roman Mezencev—removed fluid from the abdomens of the mice immediately after
injection of the cancer cells. They then added the magnetic nanoparticles to
the fluid, allowed them to mix, then magnetically removed the nanoparticles
along with the attached cancer cells before returning the fluid. The steps were
repeated six times for each mouse.
One control group received no treatment at all, while a second control group
underwent the same treatment as the experimental group—but without the magnetic
nanoparticles. Mice in the two control groups survived a median of 37 days,
while the treated mice lived 12 days longer—a 32% increase in longevity.
Though much more research must be done before the technique can be tested in
humans, McDonald and Scarberry envision a system very similar to what kidney
dialysis patients now use, but with a buffer solution circulated through the
peritoneal cavity to pick up the cancer cells.
“What we are developing is akin to hemofiltration or peritoneal
dialysis in which the patient could come into a clinic and be hooked up to the
device a couple of times a week,” said Scarberry. “The treatment is
not heavily invasive, so it could be repeated often.”
The new treatment could be used in conjunction with existing chemotherapy
and radiation. Reducing the number of free-floating cancer cells could allow a
reduction in chemotherapy, which often has debilitating side effects, Scarberry
said. The new treatment system could be used to capture spilled cancer cells
immediately after surgery on a primary tumor.
Magnetic nanoparticles suspended in a liquid are attracted to a magnet. The nanoparticles could be attached to cancer cells and then removed from the body with magnetic filtration. Credit: Gary Meek |
The researchers hope to have a prototype circulation and filtration device
ready for testing within three years. After that will come studies into the
best treatment regimen, examining such issues as the number of magnetic
nanoparticles to use, the number of treatments and treatment spacing. If those
are successful, the company will work with the FDA to design human clinical
trials.
The researchers also studying how their magnetic nanoparticles could be
engineered to capture ovarian cancer stem cells, which are not affected by
existing chemotherapy. Removing those cells could help eliminate a potent
source of new cancer cells.
The research has been supported by the Georgia Research Alliance (GRA), the
Ovarian Cancer Institute, the Robinson Family Foundation and the Deborah Nash
Harris Endowment. A member of Georgia Tech’s ATDC startup accelerator program
and a GRA VentureLab company, Sub-Micro has also raised private funding to support
its prototype development.
Challenges ahead include ensuring that nanoparticles cannot bypass the
filtration system to enter the body, and controlling the risk of infection
caused by opening the peritoneal cavity.
Beyond cancer, the researchers believe their approach could be useful for
treating other diseases in which a reduction in circulating cancer cells or
virus particles could be useful. Using magnetic nanoparticles engineered to
capture HIV could help reduce viral content in the bloodstream, for instance.
“A technology like this has many different possibilities,” said
Scarberry. “We are currently developing the technology to control the
metastatic spread of ovarian cancer, but once we have a device that can
efficiently and effectively isolate cancer cells from circulating fluids, including
blood, we would have other opportunities.”