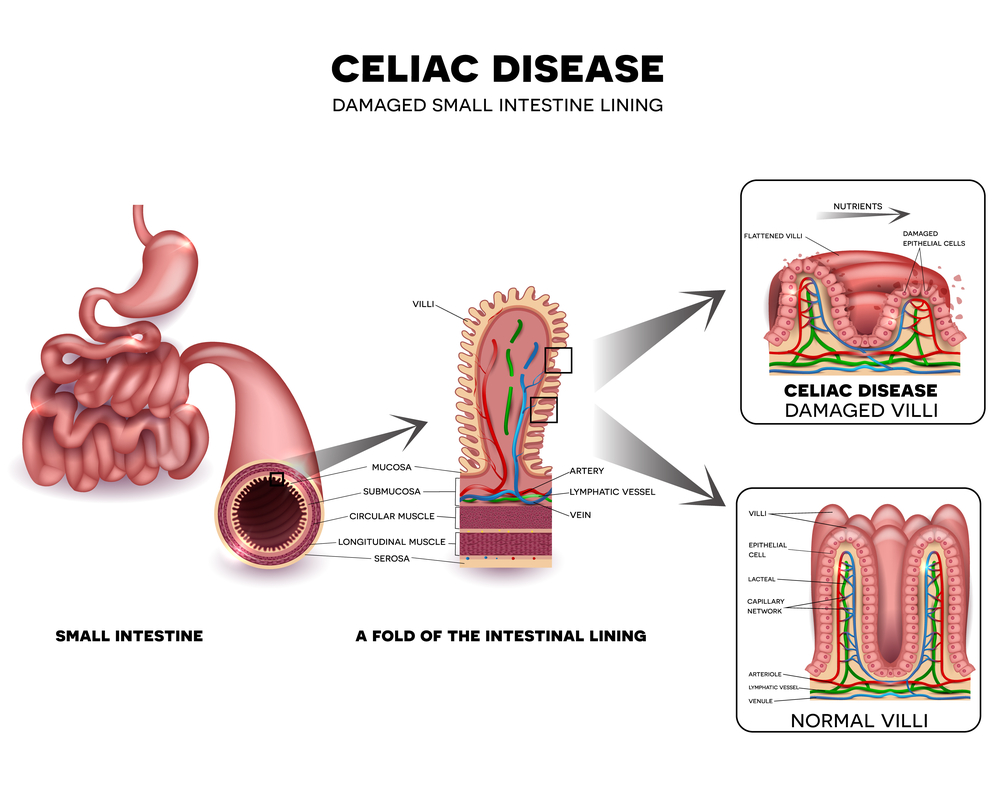
A recent study shows that even with a gluten-free diet about 20 percent of children with celiac disease still suffer from persistent intestinal damage.
For almost 20 percent of children with celiac disease persistent intestinal damage is unavoidable even with a gluten-free diet.
According to a study by MassGeneral Hospital for Children and Boston Children’s Hospital, about 19 percent of children with celiac disease sustained intestinal damage despite adherence to a strict diet.
“This study confirms that we need to look more aggressively for mucosal healing in all patients, not just adults,” Dr. Maureen Leonard, clinical director of the Center for Celiac Research and Treatment at MGHfC, said in a statement.
It is currently recommended that pediatric celiac disease patients undergo a single biopsy at diagnosis and follow-up blood testing to monitor recovery of the intestinal mucosa.
The study’s results have already been translated into revised clinical care practices at MGHfC, where most pediatric patients over the age of 10 will be monitored for mucosal healing with a repeat endoscopy, along with follow-up blood testing after one year of treatment with a gluten-free diet.
The results come on the heels of recent research in adults that showed that more than 33 percent of adult patients on a gluten-free diet have persistent intestinal damage, despite a reduction of symptoms or the results of blood tests.
While the long-term risks for children with persistent intestinal damage is not clear, adults with similar damage have been linked to an increased risk of lymphoma, low bone density and fracture. The study authors also note that “malabsorption and inflammation in children may have negative repercussions on physical and cognitive development.”
Dr. Alessio Fasano, director of the MGHfC center and co-senior author of the study, said the study results, which were based on a retrospective examination of the biopsy and medical records of 103 children with celiac treated at the two hospitals, surprised him because the children had been on the gluten-free diet for at least one year and were determined by dietitians and other hospital healthcare practitioners to have compiled well with the diet.
“The number of children who don’t heal on the gluten-free diet was much higher than what I expected,” Fasano said in a statement.
Fasano also said he was surprised that the blood levels of the autoantibody IgA tTG—the primary lab test used to monitor celiac disease—did not accurately measure mucosal recovery and neither blood test results nor patients’ symptoms accurately predicted repeat biopsy result.
The tTG antibodies that are most effective for diagnosis were not as useful for monitoring the rate of mucosal healing.
According to Fasano, this information will be used to change how celiac is treated.
“In the 1970s, pediatricians would perform three endoscopies—one at diagnosis, one after a year on the gluten-free diet and a third during the following six months, to check for healing after the patient had been re-exposed to gluten and monitored for symptoms,” Fasano said. “When we developed robust blood screening tools in the 1990s, the number of endoscopies required for standard care was reduced to one and most recently, to none in a subgroup of patients.
“We assumed that healing would occur once a patient was put on the gluten-free diet. Now that we have learned that this is not the case for all celiac patients, we are changing our clinical practice by repeating the endoscopy after one year of the implementation of the gluten-free diet.”
The study was carried out by members of the Celiac Research Program at Harvard Medical School, a collaboration between MGHfC, BCH and Beth Israel Deaconess Medical Center. As a result of the current findings, the Center for Celiac Research and Treatment at MGHfC—which treats both adults and children with celiac disease and other gluten-related disorders—plans to undertake a collaborative, prospective study on the rate of mucosal healing in children.
The study, which was published in the Journal of Pediatric Gastroenterology and Nutrition, can be viewed here.




