Researchers from the University of Michigan are developing a new pill that could help doctors accurately distinguish between benign and aggressive breast cancer tumors by making the tumors light up when exposed to infrared light.
The new technology uses a dye that responds to infrared light to tag a molecule commonly found on tumor cells in the blood vessels that feed tumors and in inflamed tissue, allowing doctors to better distinguish between a malignant cancer and a benign tumor.
Infrared light penetrates the body easily and can get to all depths of the breast without an X-ray’s small risk of disrupting DNA and seeding a new tumor. Using a dye and delivering it orally improves the overall safety of screening by reducing the possibility of severe reactions to intravenous dyes.
However, designing a pill that can carry the dye to the tumor wasn’t easy.
“To get a molecule absorbed into the bloodstream, it needs to be small and greasy. But an imaging agent needs to be larger and water-soluble. So you need exact opposite properties,” Greg Thurber, an assistant professor of chemical engineering and biomedical engineering, said in a statement.
Fortunately, they weren’t the only people looking for a molecule that could get from the digestive system to a tumor. Merck was working on a new treatment for cancer and related diseases. They got as far as phase II clinical trials demonstrating its safety, but unfortunately, it wasn’t effective.
“It’s actually based on a failed drug,” Thurber said. “It binds to the target, but it doesn’t do anything, which makes it perfect for imaging.”
In a study with mice, the researchers attached a molecule to the drug that fluoresces when it is struck with infrared light. The researchers saw the tumors light up in the mice with breast cancer that were given the drug.
The targeting molecule has already been shown to make it through the stomach unscathed, and the liver also gives it a pass, so it can travel through the bloodstream.
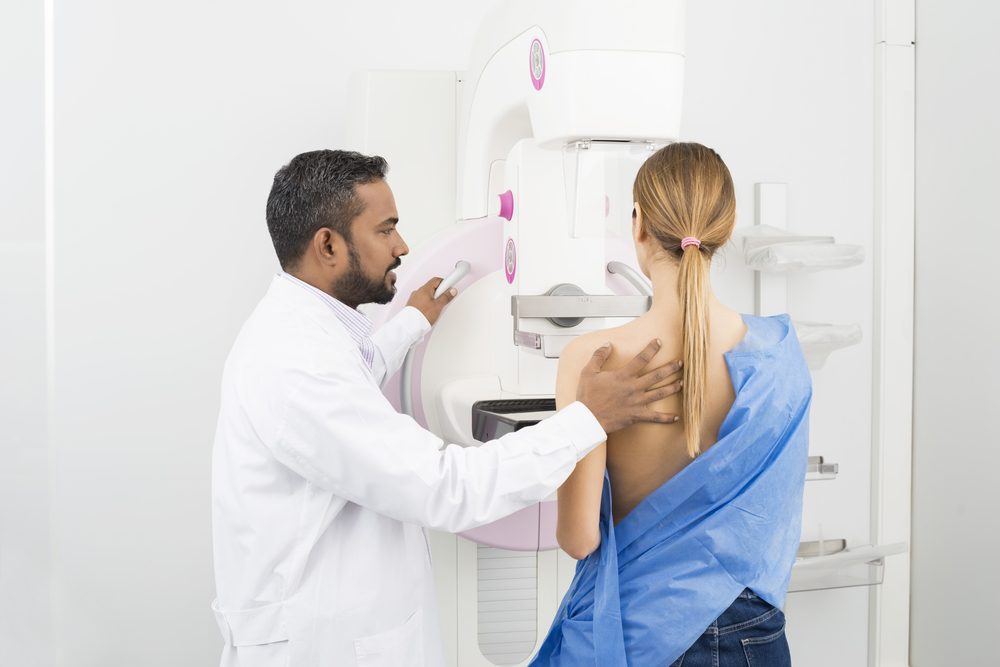
Mammography can result in overly serve treatments. About a third of breast cancer patients who are treated with surgery or chemotherapy have tumors that are benign or are so slow that they would never have become life-threatening.
Dense breast tissue can also hide the presence of lumps and results in deaths from treatable cancers.
“We overspend $4 billion per year on the diagnosis and treatment of cancers that women would never die from,” Thurber said. “If we go to molecular imaging, we can see which tumors need to be treated.”
The researchers believe the technology could also result in other cancers being identified that have previously gone undetected.
The study was published in Molecular Pharmaceutics.