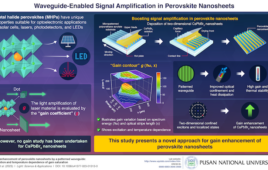
University of Utah bioengineer Rick Rabbitt using a microscope in his laboratory to study how hearing- and balance-related cells in the inner ear transmit signals to the brain. Photo Credit: Courtesy of Lee Siegel |
University
of Utah scientists used invisible infrared light to make rat heart
cells contract and toadfish inner-ear cells send signals to the brain.
The discovery someday might improve cochlear implants for deafness and
lead to devices to restore vision, maintain balance and treat movement
disorders like Parkinson’s.
“We’re
going to talk to the brain with optical infrared pulses instead of
electrical pulses,” which now are used in cochlear implants to provide
deaf people with limited hearing, says Richard Rabbitt, a professor of
bioengineering and senior author of the heart-cell and inner-ear-cell
studies published this month in The Journal of Physiology.
The
studies – funded by the National Institutes of Health – also raise the
possibility of developing cardiac pacemakers that use optical signals
rather than electrical signals to stimulate heart cells. But Rabbitt
says that because electronic pacemakers work well, “I don’t see a market
for an optical pacemaker at the present time.”
The
scientific significance of the studies is the discovery that optical
signals – short pulses of an invisible wavelength of infrared laser
light delivered via a thin, glass optical fiber – can activate heart
cells and inner-ear cells related to balance and hearing.
In
addition, the research showed infrared activates the heart cells,
called cardiomyocytes, by triggering the movement of calcium ions in and
out of mitochondria, the organelles or components within cells that
convert sugar into usable energy. The same process appears to occur when
infrared light stimulates inner-ear cells.
Infrared
light can be felt as heat, raising the possibility the heart and ear
cells were activated by heat rather than the infrared radiation itself.
But Rabbitt and colleagues did “elegant experiments” to show the cells
indeed were activated by the infrared radiation, says a commentary in
the journal by Ian Curthoys of the University of Sydney, Australia.
Curthoys
writes that the research provides “stunningly bright insight” into
events within inner-ear cells and “has great potential for future
clinical application.”
Shedding infrared light on inner-ear cells and heart cells
The
low-power infrared light pulses in the study were generated by a diode –
“the same thing that’s in a laser pointer, just a different
wavelength,” Rabbitt says.
The
scientists exposed the cells to infrared light in the laboratory. The
heart cells in the study were newborn rat heart muscle cells called
cardiomyocytes, which make the heart pump. The inner-ear cells are hair
cells, and came from the inner-ear organ that senses motion of the head.
The hair cells came from oyster toadfish, which are well-establish
models for comparison with human inner ears and the sense of balance.
Inner-ear
hair cells “convert the mechanical vibration from sound, gravity or
motion into the signal that goes to the brain” via adjacent nerve cells,
says Rabbitt.
Using
infrared radiation, “we were stimulating the hair cells, and they
dumped neurotransmitter onto the neurons that sent signals to the
brain,” Rabbitt says.
He
believes the inner-ear hair cells are activated by infrared radiation
because “they are full of mitochondria, which are a primary target of
this wavelength.”
The
infrared radiation affects the flow of calcium ions in and out of
mitochondria – something shown by the companion study in neonatal rat
heart cells.
Using an elaborate apparatus to study the inner-ear cells of the oyster toadfish (in clear plastic container, lower right), University of Utah bioengineering professor Richard Rabbitt found that infrared light similar to those in laser pointers — but at a longer and invisible wavelength — can make inner-ear “hair cells” send signals to adjacent nerve cells and then to the brain. The discovery could lead to better cochlear implants that would use infrared light rather than electrical signals to represent sounds, allowing deaf people to hear a much wider ranger of frequencies than in existing electrical implants. Photo Credit: Courtesy of Lee Siegel |
That
is important because for “excitable” nerve and muscle cells, “calcium
is like the trigger for making these cells contract or release
neurotransmitter,” says Rabbitt.
The
heart cell study found that an infrared pulse lasting a mere
one-5,000th of a second made mitochondria rapidly suck up calcium ions
within a cell, then slowly release them back into the cell – a cycle
that makes the cell contract.
“Calcium
does that normally,” says Rabbitt. “But it’s normally controlled by the
cell, not by us. So the infrared radiation gives us a tool to control
the cell. In the case of the [inner-ear] neurons, you are controlling
signals going to the brain. In the case of the heart, you are pacing
contraction.”
New possibilities for optical versus electrical cochlear implants
Rabbitt
believes the research – including a related study of the cochlea last
year – could lead to better cochlear implants that would use optical
rather than electrical signals.
Existing
cochlear implants convert sound into electrical signals, which
typically are transmitted to eight electrodes in the cochlea, a part of
the inner ear where sound vibrations are converted to nerve signals to
the brain. Eight electrodes can deliver only eight frequencies of sound,
Rabbitt says.
“A
healthy adult can hear more than 3,000 different frequencies. With
optical stimulation, there’s a possibility of hearing hundreds or
thousands of frequencies instead of eight. Perhaps someday an optical
cochlear implant will allow deaf people to once again enjoy music and
hear all the nuances in sound that a hearing person would enjoy.”
Unlike
electrical current, which spreads through tissue and cannot be focused
to a point, infrared light can be focused, so numerous wavelengths
(corresponding to numerous frequencies of sound) could be aimed at
different cells in the inner ear.
Nerve
cells that send sound signals from the ears to the brain can fire more
than 300 times per second, so ideally, a cochlear implant using infrared
light would be able to perform as well. In the Utah experiments, the
researchers were able to apply laser pulses to hair cells to make
adjacent nerve cells fire up to 100 times per second. For a cochlear
implant, the nerve cells would be activated within infrared light
instead of the hair cells.
Rabbitt
cautioned it may be five to 10 years before the development of cochlear
implants that run optically. To be practical, they need a smaller power
supply and light source, and must be more power efficient to run on
small batteries like a hearing aid.
Optical prosthetics for movement, balance and vision disorders
Electrical
deep-brain stimulation now is used to treat movement disorders such as
Parkinson’s disease and “essential tremor, which causes rhythmic
movement of the limbs so it becomes difficult to walk, function and
eat,” says Rabbitt.
He
is investigating whether optical rather than electrical deep-brain
stimulation might increase how long the treatment is effective.
Rabbitt also sees potential for optical implants to treat balance disorders.
“When
we get old, we shuffle and walk carefully, not because our muscles
don’t work but because we have trouble with balance,” he says. “This
technology has potential for restoring balance by restoring the signals
that the healthy ear sends to the brain about how your body is moving in
space.”
Optical
stimulation also might provide artificial vision in people with
retinitis pigmentosa or other loss of retinal cells – the eye cells that
detect light and color – but who still have the next level of cells,
known as ganglia, Rabbitt says.
“You
would wear glasses with a camera [mounted on the frames] and there
would be electronics that would convert signals from the camera into
pulses of infrared radiation that would be patterned onto the diseased
retina that normally does not respond to light but would respond to the
pulsed infrared radiation” to create images, he says.
Hearing
and vision implants that use optical rather than electrical signals do
not have to penetrate the brain or other nerve tissue because infrared
light can penetrate “quite a bit of tissue,” so devices emitting the
light “have potential for excellent biocompatibility,” Rabbitt says.
“You will be able to implant optical devices and leave them there for
life.”
The
heart cell study was led by Rabbitt, with University of Utah
bioengineering doctoral student Gregory Dittami as first author.
Co-authors were Suhrud Rajguru, a former Utah doctoral student now at
Northwestern University in Chicago; Utah doctoral student Richard
Lasher; and Robert Hitchcock, an assistant professor of bioengineering
at the University of Utah.
Rabbitt’s
coauthors on the inner-ear study included first author Rajguru;
Dittami; Claus-Peter Richter and Agnella Matic of Northwestern
University; neuroscientist Gay Holstein of Mount Sinai School of
Medicine in New York; and neuroscientist Stephen Highstein of the Marine
Biological Laboratory in Woods Hole, Mass.